Guide to case study nursing assignments
Info: 3014 words (12 pages) Study Guides
Published: 27 Mar 2026
Still struggling with your nursing case study? We can help! We have qualified writing experts ready to assist, check out the nursing assignment help section for more details.
Case study assignments in nursing are designed to bridge the gap between theoretical knowledge and clinical practice. They present student nurses with detailed patient scenarios, often based on real or simulated clinical situations, and require analysis of the patient’s problems, formulation of nursing interventions, and consideration of outcomes.
These assignments test not only nursing knowledge but also critical thinking and decision-making skills. Indeed, case studies facilitate active learning and encourage the development of clinical reasoning (Popil, 2011).
By working through a realistic case, students learn to apply nursing theory to practice and to justify their care decisions with evidence. This guide provides a comprehensive approach to analysing nursing case studies, from understanding the scenario and identifying priority issues to planning interventions and evaluating patient outcomes. It also offers tips on structuring your assignment and ensuring a high-quality, evidence-based analysis.
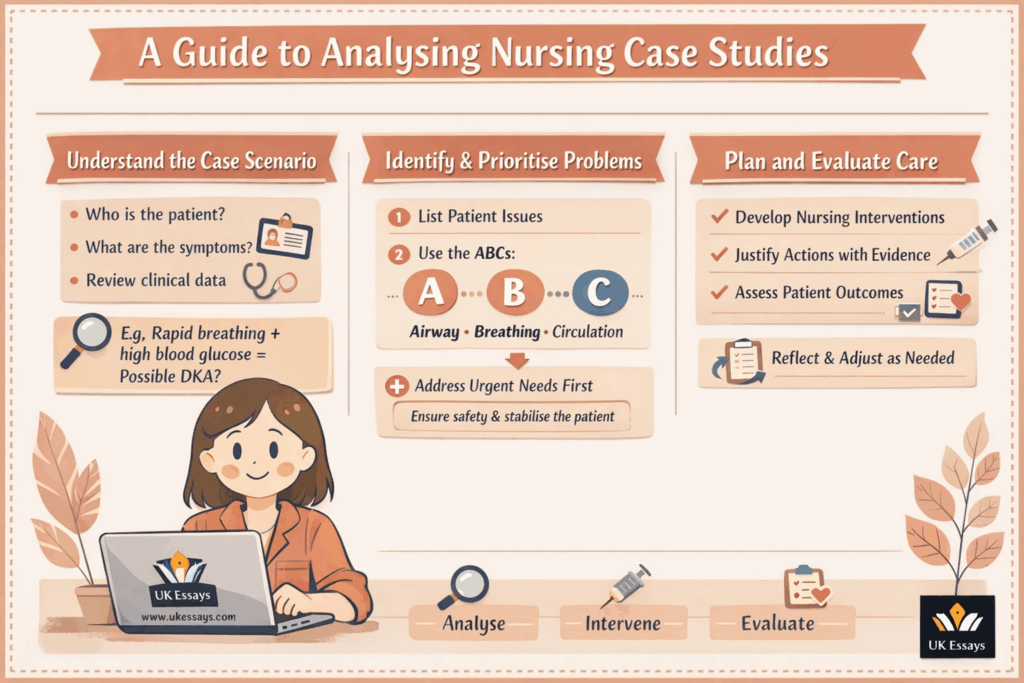
Understanding the case scenario
Before rushing into writing, carefully read the case scenario provided. Start by identifying the key patient details. Who is the patient in terms of age, gender, and background? Why have they presented to care, and what are their primary symptoms or concerns?
Take note of vital signs, medications, test results, or any other clinical data. These details often contain clues about underlying problems.
For example, a case study might describe a patient with rapid breathing, fruity-scented breath, abdominal pain, and very high blood glucose. Even if it is not explicitly stated, these cues point towards diabetic ketoacidosis (DKA) as the likely problem.
In a case study assignment, you are expected to infer such clinical issues from the information given. This demonstrates your ability to interpret data and recognise patterns.
Therefore, scrutinise the scenario for signs, symptoms, and context, such as recent illnesses or medication omissions, that help you form a preliminary picture of the patient’s situation. It can be useful to jot down the patient’s problems or potential diagnoses as you read. This will guide your subsequent analysis.
Identifying problems and prioritising needs
Once you understand the scenario, the next step is to pinpoint the patient’s health problems or nursing diagnoses. These may be overt, such as pain or shortness of breath, or more subtle, such as anxiety or risk of infection, depending on the case details.
List all the relevant problems or issues affecting the patient’s health. Then prioritise them to decide which ones need urgent attention and which are secondary.
In nursing, a common approach is to use the ABC framework: Airway, Breathing, Circulation. This means addressing immediate life-threatening issues first (Resuscitation Council UK, 2024).
For instance, in a DKA case, airway and breathing would be assessed immediately. An altered level of consciousness or very rapid breathing could compromise ventilation. Circulation, including shock or dehydration, would be the next priority. After stabilising ABC, you would address other concerns such as pain, the underlying cause of DKA, and so on.
Prioritisation should be logical and justified. Explain why one issue is managed before another. For example, maintaining airway patency and adequate breathing is the top priority because, without oxygenation, the patient is at risk of cardiac arrest.
This demonstrates clinical reasoning. It also helps structure your analysis, as you can discuss the case in order of urgency or importance.
Applying theoretical knowledge to practice
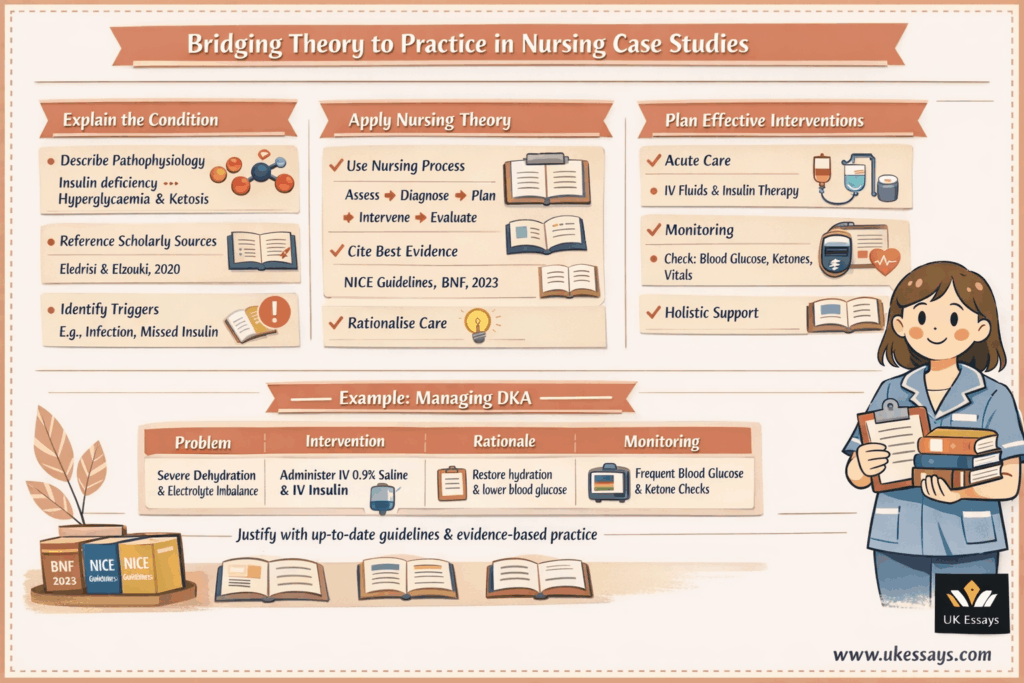
A high-quality case study analysis goes beyond describing the patient’s signs and listing problems. It links theory to practice throughout the discussion.
This means explaining the pathophysiology behind the patient’s condition, referencing relevant research or guidelines, and showing understanding of best practice. Ask yourself: what underlying condition or concept explains this patient’s presentation, and what do I know about it?
In our DKA example, you would briefly explain how insulin deficiency and counter-regulatory hormones lead to hyperglycaemia, ketone production, dehydration, and acidosis. Incorporate scholarly sources to support this explanation, such as textbooks or journal articles on the disease process.
For instance, you might note that DKA is characterised by high blood glucose, metabolic acidosis, and ketones. It is often precipitated by infection or missed insulin doses (Eledrisi and Elzouki, 2020). By doing so, you show your markers that you understand why the patient has these symptoms and lab results.
Using nursing frameworks
Relating the case to nursing theory or models can strengthen your analysis. You might apply the nursing process of assessment, diagnosis, planning, implementation, and evaluation as an organising framework. You could also draw on clinical reasoning models taught in your programme.
The crucial element is to show that you can interpret the patient’s story through the lens of nursing knowledge and evidence-based practice.
Remember that every claim or clinical inference in your assignment should be backed by evidence or sound rationale. Nursing education places strong emphasis on evidence-based practice. The Nursing and Midwifery Council (NMC) Code requires nurses to use “best available evidence” in making care decisions (NMC, 2018).
Therefore, ensure you cite up-to-date clinical guidelines or research to justify each major point, whether it is a normal reference range for a lab result or the recommended treatment for a condition.
Planning nursing interventions
After identifying the patient’s problems and understanding their causes, the core of a case study assignment is to propose appropriate nursing interventions. These are the actions the nurse, or wider healthcare team, should take to address the patient’s needs.
For each problem on your list, ask: what can a nurse do to improve or resolve this issue, and how exactly will it help the patient? Answering this will form the basis of your care plan.
It is helpful to structure this section problem by problem or in order of priority. For each identified issue, state the intervention and then provide a rationale explaining why it is needed and how it works. Always link back to evidence or guidelines so your interventions are grounded in professional best practice.
Acute interventions and rationale
For example, continuing with the DKA scenario, if one problem is severe dehydration and electrolyte imbalance, a primary intervention is to commence urgent intravenous fluid and insulin therapy.
According to the British National Formulary, the treatment of DKA aims to restore circulatory volume, correct electrolyte imbalance and hyperglycaemia, clear ketones, and suppress ketone production (BNF, 2023).
You would therefore explain that giving IV 0.9% saline rehydrates the patient and improves perfusion. An insulin infusion will gradually lower blood glucose and stop further ketone accumulation.
You should also mention monitoring tasks, such as frequent blood glucose and ketone checks, electrolyte monitoring, and vital signs, as interventions. Close observation is a key nursing action in acute cases.
Each intervention must directly relate to a problem identified earlier and should be specific. Rather than saying “improve breathing”, you might say “administer oxygen at 15 L/min via a non-rebreather mask if oxygen saturation is below target, to treat hypoxia.”
Holistic care needs
Make sure to consider holistic care needs too, not only the physiological ones. Address pain management, psychosocial support, patient safety, and patient education where appropriate.
For a patient admitted with DKA, once emergent issues are managed, education becomes crucial. Teaching the patient about insulin adherence, blood glucose monitoring, and sick-day rules will help prevent future episodes (Eledrisi and Elzouki, 2020).
By covering physiological, psychological, and educational interventions, you demonstrate comprehensive nursing care. Use clinical guidelines, such as national diabetes guidelines or hospital protocols, to support your intervention choices wherever possible.
Setting goals and expected outcomes
As part of planning interventions, it is good practice to specify the goals or expected outcomes for each intervention. In other words, how will you know if the intervention is successful?
In case study assignments, you may not always be explicitly asked to include a formal care plan with goals. However, including outcome criteria shows a higher level of clinical thinking.
For example, if one intervention is fluid resuscitation for the DKA patient, the expected outcome could be that the patient’s blood pressure will stabilise above 100 mmHg systolic and urine output will be at least 0.5 mL/kg/hour, indicating adequate perfusion. If you administer oxygen for hypoxia, an outcome could be that oxygen saturation will improve to 94% or above on oxygen.
Stating outcomes in measurable terms, such as pain score reduction, respiratory rate normalising, or the patient verbalising understanding of insulin use, makes the evaluation clearer. It also aligns with the nursing process, especially the planning and evaluation stages.
When writing the assignment, you can integrate these expected outcomes into your discussion. For example, you might write: “Intravenous morphine 2 mg was administered to address the patient’s severe abdominal pain. The goal was to reduce the pain from 9/10 to below 3/10 within 30 minutes.”
This approach links the intervention with its purpose and anticipated result. It shows that you are thinking ahead to how you would evaluate the patient’s response, which is exactly what nurses must do in practice.
Evaluation and reflection on outcomes
Many case study assignments will ask you to discuss or hypothesise about the patient’s progress after interventions, in other words, they ask you to evaluate outcomes.
In a real clinical setting, evaluation is the step where you observe whether the patient’s condition has improved and decide on next steps. In an assignment, you may not have actual patient outcomes. Even so, you can discuss likely outcomes based on evidence or the literature.
For each major intervention you propose, consider what improvement you would expect and what follow-up actions may be needed. For example, after initiating fluids and insulin in DKA, you would expect the patient’s blood glucose to fall gradually and ketone levels to clear over several hours. You would also watch for complications such as hypoglycaemia or hypokalaemia during this process and adjust treatment as needed.
If an intervention did not achieve the expected effect, mention what alternative or additional actions could be taken. Perhaps the patient’s blood pressure remains low despite fluids. You might then consider whether vasopressors are needed, or whether an underlying infection should be identified and treated.
Reflection and learning
This demonstrates adaptability in clinical reasoning. Case study analyses can also benefit from a brief reflection on what was learned or what the nurse could do better.
This might include recognising early signs that were initially missed or acknowledging the importance of teamwork and communication. Reflective thinking shows that you understand nursing is a continuous learning process.
However, keep reflections concise and relevant to the case. The main focus should remain on clinical analysis rather than personal feelings.
If the assignment specifically asks for a personal reflection, you can include a separate reflective paragraph or conclusion. Otherwise, a sentence or two about lessons from the scenario or implications for future practice is enough to give a professional rounding-off to your discussion.
Structuring your case study assignment
A clear, logical structure is crucial for readability and for meeting academic requirements. Generally, your case study assignment should be organised into an introduction, main body, and conclusion, with headings for major sections if allowed. Always follow your assignment brief or school guidelines on formatting.
Write the introduction so it summarises the case scenario and states what your analysis will cover. For example, introduce the patient’s situation briefly, such as “This case study examines an adult patient with type 2 diabetes admitted in diabetic ketoacidosis…”. Then present a thesis or overview of your approach, such as “The analysis identifies the patient’s primary clinical priorities and outlines evidence-based nursing interventions to stabilise her condition and prevent recurrence.”
The introduction should be concise but informative. It sets the stage for the reader.
Organising the main body
In the main body, use either thematic headings, such as by problem, or a chronological approach that moves from assessment findings to interventions and then evaluation. Ensure each paragraph has a clear point.
For instance, one paragraph might discuss the assessment and immediate management of dehydration in DKA. The next might deal with electrolyte correction and monitoring.
Use transitional words and phrases to maintain flow between paragraphs and ideas. Examples include “furthermore”, “in addition”, and “however”. These guide the reader through your reasoning and make the text more cohesive.
Writing style and conclusion
Throughout, write in an academic yet accessible style. Avoid colloquial language, but explain clinical terms if needed for clarity. Write in the active voice where possible. For example, say “The nurse will monitor the patient’s level of consciousness hourly” rather than “Hourly monitoring of the level of consciousness will be done”.
Your assignment should end with a conclusion that succinctly recaps the main points of your analysis. Do not introduce new information there. Instead, summarise how the patient’s key issues were managed and the expected outcomes.
You might also briefly mention the broader significance. For instance, you could note how the case study illustrates the importance of prompt assessment and evidence-based intervention in achieving good patient outcomes.
A strong concluding statement could be: “In summary, this case study has demonstrated how systematic nursing assessment and priority-driven interventions can successfully manage a complex clinical condition like diabetic ketoacidosis, ultimately improving patient safety and prognosis.”
Ensuring quality and academic rigor
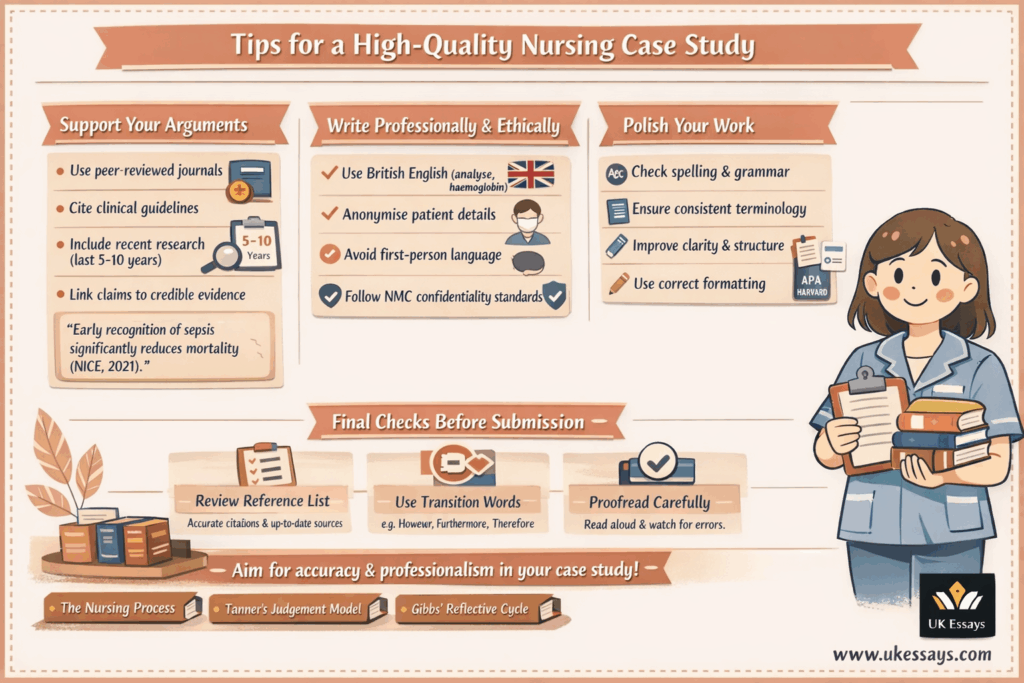
Finally, to elevate your case study assignment to an exceptional level, pay attention to detail in both content and presentation.
Support all critical points with evidence. This cannot be overstated. In academic and clinical writing, unsubstantiated claims weaken credibility. Use high-quality sources such as clinical guidelines, nursing textbooks, and peer-reviewed journals.
For example, if you assert that early recognition and management of sepsis in a case study is vital, back it up with a reference to sepsis guidelines or a study on sepsis outcomes.
Evidence, referencing, and ethics
All sources should be cited in-text in Harvard style, using the Author and Year format, and listed in a reference list at the end. Ensure your references are recent whenever possible. As a general rule, prioritise research or guidelines from the last 5 to 10 years unless you are citing a seminal work.
Present the reference list in proper Harvard format, alphabetically by author or organisation.
Because you are writing in British English, double-check that spelling and terminology are consistent. Use “analyse” rather than “analyze”, and “haemoglobin” rather than “hemoglobin”.
Maintain a formal tone and avoid first person unless the assignment explicitly allows personal reflection. It is also important to consider ethical and professional guidance. If your case study is based on a real patient you encountered, anonymise the patient’s details in line with confidentiality standards (NMC, 2018). This shows awareness of professional ethics even in academic work.
Final checks before submission
Before submission, revise and proofread your assignment carefully. Look for any sections that might be unclear and refine them for clarity.
Verify that the logical flow is smooth and that each section connects to the next. For example, if you mention a lab result in the assessment section, make sure you later discuss its relevance when planning interventions.
Check sentence structure to minimise passive phrasing and long, convoluted sentences. Variety in sentence length can make the text more engaging, but clarity must remain the priority.
Additionally, use transition words to improve flow. Words such as “however”, “therefore”, “consequently”, “moreover”, and “for example” help signal the relationship between ideas and guide the reader.
Lastly, consider the overall presentation. Make sure headings are used appropriately and formatted in sentence case, paragraphs are not overly long, and any required formatting, such as line spacing or font size, meets the assignment criteria. A well-structured and polished assignment creates a strong impression of diligence and professionalism.
Conclusion
Case study nursing assignments are an invaluable exercise in applying theory to practice. They challenge students to think like nurses, to gather cues from patient information, identify what is happening, decide on priorities, take action, and anticipate the results.
By following a structured approach like the one outlined in this guide, you can break down a complex clinical scenario into manageable parts. Start with a thorough understanding of the case, then use your nursing knowledge to analyse the patient’s problems and plan evidence-based interventions.
Always justify your decisions with rationales and references, demonstrating critical thinking and adherence to best practice. Through clear organisation and rigorous content, your case study analysis will showcase your ability to deliver safe, effective nursing care on paper. This ultimately reflects your readiness for real-world clinical situations.
By honing these skills, including problem identification, prioritisation, intervention planning, and outcome evaluation, you not only improve your assignments but also lay the groundwork for sound clinical judgement in your future career.
In essence, a well-executed case study assignment is more than an academic task. It is a rehearsal of professional practice, preparing you to provide high-quality, evidence-based care to patients.
Further reading
One useful area for further reading is the nursing process itself. Looking more closely at assessment, diagnosis, planning, implementation, and evaluation can help you structure case study work more confidently and logically.
You may also find Tanner’s Clinical Judgement Model helpful. It expands your understanding of how nurses notice cues, interpret information, respond appropriately, and reflect on outcomes in practice.
Another relevant framework is Gibbs’ Reflective Cycle. While case study assignments are mainly analytical, this model can strengthen any reflective element by helping you think clearly about what was learned and how future practice could improve.
Still struggling with your nursing case study? We can help! We have qualified writing experts ready to assist, check out the nursing assignment help section for more details.
References
- British National Formulary (BNF) (2023) Diabetic hyperglycaemic emergencies. London: BMJ Group and Pharmaceutical Press. (Accessed via NICE Medicines Complete).
- Eledrisi, M.S. and Elzouki, A.N. (2020) ‘Management of diabetic ketoacidosis in adults: A narrative review’, Saudi Journal of Medicine & Medical Sciences, 8(3), pp. 165–173.
- Nursing & Midwifery Council (NMC) (2018) The Code: Professional standards of practice and behaviour for nurses, midwives and nursing associates. London: NMC.
- Popil, I. (2011) ‘Promotion of critical thinking by using case studies as teaching method’, Nurse Education Today, 31(2), pp. 204–207.
- Resuscitation Council UK (2024) The ABCDE Approach (Guidance for managing critically ill patients). London: RCUK. (Updated July 2024).
Cite This Work
To export a reference to this article please select a referencing stye below:



